Most people do not realize they have gum disease until a dentist tells them. That is not because the signs are invisible — it is because gum disease rarely causes pain in its early stages, and it is easy to dismiss symptoms like occasional bleeding or mild sensitivity as normal. They are not. Your gums should not bleed when you brush. They should not be tender to the touch. And if your breath is not improving with regular brushing, that is worth paying attention to.
Gum disease is the leading cause of tooth loss in adults. It is also one of the most preventable conditions in dentistry. Catching it early — before it progresses from gingivitis to periodontitis — makes treatment dramatically simpler, less invasive, and less expensive. This guide walks through the warning signs Oceanside patients should know, what causes gum disease to develop, and what treatment looks like when you catch it at different stages.
What Is Gum Disease?
Gum disease is an infection of the tissues that surround and support your teeth. It starts with bacteria in plaque, the sticky film that forms on teeth throughout the day. When plaque is not removed consistently through brushing and flossing, it hardens into tartar, which can only be removed by a dental professional. The bacteria in tartar irritate the gum tissue, causing inflammation that, over time, can spread beneath the gum line and begin destroying the bone that holds your teeth in place.
There are two main stages:
- Gingivitis is the early stage. Gums are inflamed, may bleed easily, and can appear red or swollen. At this stage, no permanent damage has occurred. Gingivitis is fully reversible with professional cleaning and improved home care.
- Periodontitis is the advanced stage. The infection has spread below the gum line and is actively breaking down the bone and connective tissue that anchor your teeth. This damage cannot be fully reversed, but it can be stopped and managed with the right treatment.
The gap between these two stages is often years — which is exactly why regular dental exams in Oceanside matter so much. Most patients who develop periodontitis had clear warning signs long before the damage became serious.
8 Warning Signs of Gum Disease You Should Not Ignore
1. Bleeding Gums When You Brush or Floss
This is the most common early sign and the one most often dismissed. Many people assume their gums bleed because they brush too hard or have not been flossing regularly. While inconsistent flossing can cause temporary sensitivity, persistent bleeding is a sign of inflammation — not technique. Healthy gums do not bleed during normal brushing and flossing. If yours do, it is worth having them evaluated.
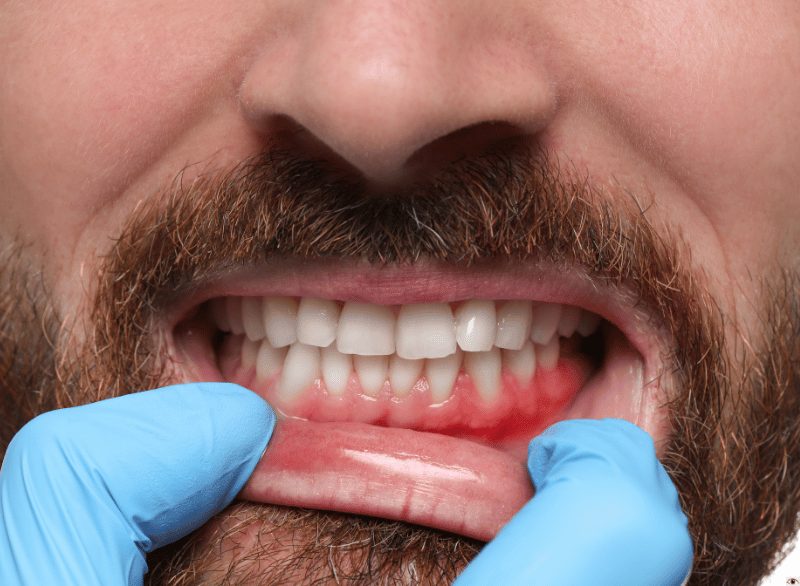
2. Swollen, Red, or Tender Gums
Healthy gum tissue is firm and pale pink. Gums that are puffy, red, or sensitive to touch are inflamed — the body’s response to bacterial infection. This is gingivitis presenting itself visually. At this stage, a professional cleaning and improved home care routine can reverse the damage entirely.
3. Persistent Bad Breath
Bad breath that does not respond to brushing, flossing, or mouthwash is one of the more telling signs of gum disease. The bacteria responsible for periodontal infections produce sulfur compounds that cause a persistent, unpleasant odor. If you or someone around you notices that your breath is consistently off despite good hygiene habits, gum disease should be on the list of things to rule out.
4. Receding Gum Line
If your teeth appear longer than they used to, or if you can see more of the tooth root near the gum line, your gums are receding. Recession can result from gum disease, aggressive brushing, or a combination of both. Beyond the cosmetic concern, recession exposes root surfaces that are more vulnerable to decay and sensitivity. Gum recession treatment in Oceanside is most effective when addressed early, before significant tissue loss occurs.
5. Loose or Shifting Teeth
Adult teeth should not move. If you notice any looseness, shifting, or changes in how your teeth fit together when you bite, the supporting bone around those teeth may have been compromised by periodontitis. This is a sign of advanced disease and requires prompt attention. The longer it goes untreated, the higher the risk of tooth loss.
6. Sensitive Teeth Along the Gum Line
Sensitivity to hot, cold, or sweet foods along the gum line — rather than in the center of a tooth — often indicates root exposure from recession. When gum tissue pulls back, the root surface is left unprotected. This type of sensitivity is frequently a symptom of gum disease rather than a cavity or enamel issue, and treating the underlying gum problem is the right first step.
7. Pus Between Teeth and Gums
The presence of pus anywhere in the mouth is a sign of active infection. Pus between teeth and gums indicates a periodontal abscess — a pocket of bacteria that has become trapped and is causing a localized infection. A periodontal abscess requires prompt treatment. If you notice swelling, a bad taste in your mouth, or visible discharge near the gum line, call Streelman DDS in Oceanside as soon as possible. This is not something to wait on.
8. Pain When Chewing
Discomfort when biting or chewing can indicate that infection has progressed deeper into the supporting structures of the tooth. While pain is not always present with gum disease, when it does appear it typically signals a more advanced stage. Do not assume chewing discomfort is a cavity — have a dentist evaluate whether the gum tissue and bone around the affected tooth are involved.
What Causes Gum Disease?
Plaque buildup is the primary driver, but several factors can accelerate how quickly gum disease develops and how severe it becomes:
- Infrequent or insufficient brushing and flossing allows plaque to accumulate and harden into tartar
- Smoking and tobacco use significantly increases risk and makes treatment less effective by impairing the body’s ability to fight infection
- Uncontrolled diabetes is closely linked to periodontal disease — the relationship goes both ways, with each condition making the other harder to manage
- Certain medications that cause dry mouth reduce saliva flow, which plays a key role in washing bacteria off teeth and gum tissue
- Hormonal changes during pregnancy, puberty, or menopause can make gums more susceptible to inflammation
- Genetics plays a role — some patients are simply more prone to gum disease regardless of how diligent they are with their hygiene routine
- Skipping dental cleanings means tartar goes unremoved, giving bacteria a persistent foothold below the gum line
Understanding your personal risk factors is part of what Dr. Streelman reviews at every comprehensive exam. If you have one or more of these factors, more frequent professional cleanings may be appropriate for your situation.
How Gum Disease Is Treated in Oceanside
Treatment depends on how far the disease has progressed when it is caught. This is the core reason early detection matters so much — the treatment options at the gingivitis stage are simple and painless compared to what is required for advanced periodontitis.
Gingivitis: Professional Cleaning and Home Care
At the earliest stage, a thorough professional cleaning to remove plaque and tartar, combined with an improved brushing and flossing routine at home, is often all that is needed to fully reverse the condition. This is why preventive dental care in Oceanside is the most cost-effective investment you can make in your oral health.
Moderate Gum Disease: Scaling and Root Planing
When the disease has progressed beyond the gum line, a deep cleaning procedure called scaling and root planing is the first-line treatment. This involves removing plaque and tartar from below the gum line and smoothing the root surfaces of the teeth so that gum tissue can reattach. The procedure is performed under local anesthetic and is well tolerated by most patients. For patients who feel anxious about dental procedures, sedation dentistry options are available at Streelman DDS that make deep cleaning significantly more comfortable.
Advanced Gum Disease: Periodontal Maintenance and Ongoing Care
Once active gum disease has been treated, ongoing periodontal maintenance appointments — typically every three to four months — are essential to prevent recurrence. At these visits, Dr. Streelman and his team clean below the gum line, measure pocket depths, and monitor for any signs the infection is returning. Patients who stay consistent with maintenance have significantly better long-term outcomes than those who return to a standard six-month cleaning schedule too soon.
More advanced cases involving significant bone loss or deep pockets may require a referral to a periodontist. Dr. Streelman will be direct with you about what level of care is most appropriate for your specific situation.
Why Gum Disease Affects More Than Your Mouth
Research has established meaningful links between periodontal disease and serious systemic health conditions. The bacteria involved in gum infections can enter the bloodstream and trigger inflammatory responses elsewhere in the body. Studies have found associations between untreated gum disease and an increased risk of heart disease, stroke, poorly controlled type 2 diabetes, respiratory infections, and complications during pregnancy.
This does not mean gum disease causes these conditions directly — the relationship is complex and still being studied. But it does mean that treating gum disease is not just about saving teeth. It is part of a broader picture of overall health. At Streelman DDS in Oceanside, we take that connection seriously.
How to Prevent Gum Disease
The good news is that gum disease is largely preventable. The habits that prevent it are simple and well established:
- Brush thoroughly twice a day, paying attention to the gum line
- Floss at least once daily to remove plaque from between teeth where a toothbrush cannot reach
- Schedule professional cleanings every six months, or more frequently if recommended
- Do not smoke or use tobacco products
- Manage systemic health conditions like diabetes that increase your risk
- Stay hydrated to support healthy saliva flow
If it has been more than six months since your last cleaning, or if you have noticed any of the warning signs described in this post, the right move is to schedule an evaluation. Early treatment is always simpler than late treatment. Book an appointment at Streelman DDS in Oceanside today.
Frequently Asked Questions About Gum Disease
Can gum disease go away on its own?
Gingivitis can be reversed with professional cleaning and improved home care, but it will not resolve on its own without intervention. More advanced gum disease requires professional treatment and will worsen over time if left unaddressed.
Is gum disease painful?
Not usually, especially in the early stages. This is part of what makes it easy to miss. Pain, when it occurs, typically indicates a more advanced stage or an acute infection such as a periodontal abscess.
How do I know if I have gum disease or just sensitive gums?
The only reliable way to know is a periodontal evaluation with pocket depth measurements and X-rays. Sensitivity, bleeding, and tenderness can all have other causes, but they can also be signs of gum disease. A professional exam rules out or confirms the diagnosis.
Can gum disease affect my overall health?
Research has found associations between untreated periodontal disease and conditions including heart disease, stroke, diabetes complications, and pregnancy complications. Treating gum disease is an investment in overall health, not just dental health.
How often should I get a dental cleaning if I have had gum disease?
Most patients who have been treated for gum disease benefit from periodontal maintenance appointments every three to four months rather than the standard six-month interval. The frequency depends on how well the condition is responding to treatment and how deep the remaining pockets are.
Does sedation dentistry help with gum disease treatment?
Yes. Many patients who have avoided the dentist due to anxiety find that sedation dentistry makes procedures like scaling and root planing much more manageable. Dr. Streelman offers oral sedation, IV sedation, and nitrous oxide at his Oceanside practice. Ask about your options when you call to schedule.
What is a periodontal abscess and is it an emergency?
A periodontal abscess is a localized pocket of infection in the gum tissue. It typically causes sudden pain, swelling, and a bad taste in the mouth. It should be treated promptly — call Streelman DDS at (760) 439-0600 if you suspect you have one. Delaying treatment allows the infection to spread.
Ready to have your gums evaluated? Schedule an appointment at Streelman DDS in Oceanside, CA. Dr. Streelman and his team will assess your gum health, walk you through what they find, and give you a clear plan with no surprises.
